Nodal marginal zone lymphoma
This information is about nodal marginal zone lymphoma – a rare, slow-growing type of non-Hodgkin lymphoma.
On this page
What is nodal marginal zone lymphoma?
What is nodal marginal zone lymphoma?
Lymphoma is a type of blood cancer that develops when white blood cells called lymphocytes grow out of control. Lymphocytes are part of your immune system. They travel around your body in your lymphatic system, helping fight infections. There are two types of lymphocyte: B lymphocytes (B cells) and T lymphocytes (T cells).
Lymphomas can be grouped as Hodgkin lymphomas or non-Hodgkin lymphomas, depending on the types of cell they contain. Marginal zone lymphomas are types of slow-growing (low-grade) non-Hodgkin lymphomas that develop from B cells. They are called marginal zone lymphomas because they develop in a particular region found at the edge of normal lymphoid tissues (collections of lymphocytes) called the marginal zone.
There are three types of marginal zone lymphoma:
- nodal marginal zone lymphoma, which develops in lymph nodes
- MALT lymphoma (also known as extranodal marginal zone lymphoma), which develops in lymphoid tissue outside lymph nodes
- splenic marginal zone lymphoma, which develops in the spleen.
Nodal marginal zone lymphoma (often called nodal MZL or NMZL) develops when abnormal B cells collect in your lymph nodes.
What are lymph nodes?
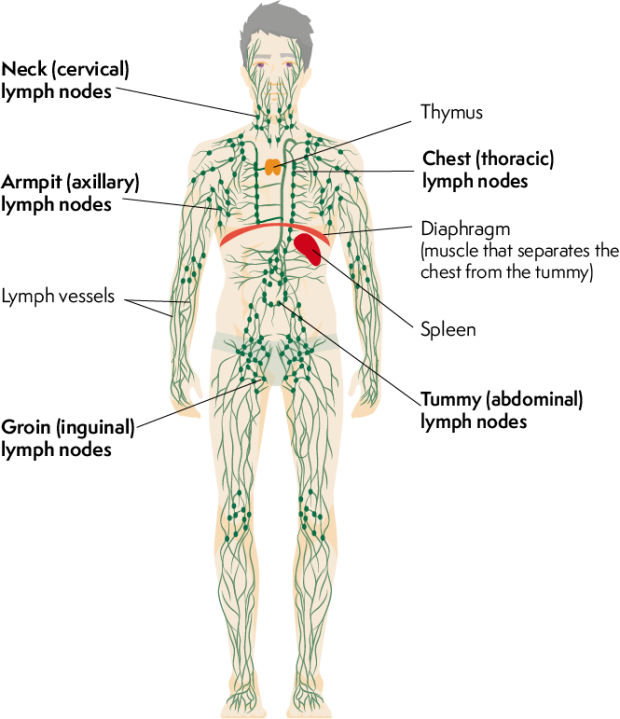
Lymph nodes are pea-sized glands, or lumps, that are part of your immune system. They are used by your body to remove bacteria and other harmful cells. There are hundreds of lymph nodes found throughout the body, with clusters in your neck, armpits, chest, abdomen (tummy) and groin.
Who gets nodal marginal zone lymphoma?
Nodal MZL is rare. It accounts for fewer than 2 in every 100 cases of non-Hodgkin lymphoma. Nodal MZL can affect people of any age but it is most common in people over 50.
In most cases, it is not known what causes nodal MZL. It is more common in people who have been infected with hepatitis C virus and some autoimmune conditions. However, the vast majority of people who have had hepatitis C or autoimmune conditions do not go on to develop lymphoma.
There is a very rare paediatric variant of nodal MZL that affects children. This typically develops in lymph nodes in the head and neck. It is usually diagnosed at an early stage and has an excellent outlook.
Symptoms of nodal marginal zone lymphoma
The most common symptom of nodal MZL is swollen lymph nodes, typically in the neck. The lumps are not usually painful. Lymph nodes in several parts of the body are often affected. This might include lymph nodes inside your chest or tummy, where you can’t feel them.
You might not have any other symptoms. Some people experience unexplained weight loss, night sweats or fever. These are known as ‘B symptoms’ and often occur together.
Some people feel very tired, especially if the lymphoma has affected the bone marrow and is causing anaemia.
Diagnosis and staging of nodal marginal zone lymphoma
Nodal MZL can be difficult to diagnose because it can look similar to other types of lymphoma. It is usually diagnosed by removing a swollen lymph node, or a sample of cells from one, and looking at it under a microscope. This involves a small procedure called a biopsy, which is usually done under local anaesthetic. The biopsy sample is examined by an expert pathologist. The pathologist also tests the sample for particular proteins that are found on the surface of lymphoma cells. This can help your medical team decide on the most appropriate treatment for you based on your lymphoma diagnosis.
You also have blood tests to look at your general health, check your blood cell counts, make sure your kidneys and liver are working well and test for infections such as hepatitis C virus.
You have other tests to find out which areas of your body are affected by lymphoma. This is called staging. This usually involves having a CT scan. You might also have a PET scan, although this is less common for marginal zone lymphomas than other types of lymphoma. You might have a sample of your bone marrow cells collected (a bone marrow biopsy) to check if you have lymphoma cells in your bone marrow.
You usually have your tests done as an outpatient. It takes a few weeks to get all the results. Waiting for test results can be a worrying time, but it is important for your doctor to gather all of this information in order to plan the best treatment for you.
Nodal MZL is often advanced (stage 3 or 4) by the time it is diagnosed. About 1 in 3 people with nodal MZL have lymphoma cells in their bone marrow. Effective treatment is available for advanced nodal MZL.
Outlook for nodal marginal zone lymphoma
Nodal MZL develops slowly. Treatment is often successful, but the lymphoma often relapses (comes back) and needs more treatment to keep it under control. Most people live with this type of lymphoma for many years. You might have times when you feel well and don’t need treatment, and other times when your symptoms get worse and you need more treatment.
Your doctor is best placed to advise you on your outlook based on your individual circumstances.
Transformation
Occasionally, nodal MZL can change (transform) into a faster-growing type of lymphoma. This happens in less than 2 in every 10 people with nodal MZL.
If your doctor thinks your lymphoma might have transformed, you will usually have a biopsy to check for faster-growing cells and a PET/CT scan to see which areas of your body are affected. Transformed nodal MZL lymphoma is treated in the same way as fast-growing (high-grade) non-Hodgkin lymphoma, such as diffuse large B-cell lymphoma (DLBCL).
Treatment of nodal marginal zone lymphoma
The treatment you have for nodal MZL depends on how the lymphoma is affecting you, the stage it is at and your general health.
If you have hepatitis C virus, you are likely to be offered anti-viral treatment. Clearing the infection might also clear the lymphoma. If this is the case, you might not need any more treatment.
Active monitoring
If your lymphoma is not causing troublesome symptoms, you might not need treatment straightaway. Instead, your doctor might suggest monitoring you closely and saving treatment until it is needed. This is called active monitoring or ‘watch and wait’. This approach allows you to avoid the side effects of treatment for as long as possible. Delaying treatment in this way does not affect how well it works when you do need it, or how long you might live.
Early stage nodal MZL
If you need treatment and you only have lymphoma in one or a few places close together, you might have radiotherapy. However, most people with nodal MZL have more widespread lymphoma.
Because the lymphoma was confined to my neck, armpit and just above my collar bone, the medical team felt that radiotherapy would be appropriate.
Read more about Julian’s story.
Advanced stage nodal MZL
The most likely treatment for people with advanced stage nodal MZL is antibody therapy (such as rituximab) combined with chemotherapy. This is called ‘chemo-immunotherapy’.
Nodal MZL is rare. This makes it difficult to determine exactly which treatment gives the best outcome. The most common combinations of chemo-immunotherapy drugs used to treat nodal MZL are:
- rituximab plus bendamustine
- rituximab plus chlorambucil
- rituximab plus CVP (R-CVP)
- rituximab plus CHOP (R-CHOP).
However, your doctor might recommend a different regimen (combination of drugs), or they might ask if you’d like to take part in a clinical trial.
If you have had successful chemo-immunotherapy, your doctor may recommend rituximab as a maintenance therapy. Maintenance rituximab is usually given by a subcutaneous (under the skin) injection every 2 to 3 months for up to 2 years. Maintenance therapy may prolong the length of your remission. Your doctor will discuss the potential risks and benefits of maintenance rituximab if this is an option for you.
Side effects of treatment
Treatments affect people differently. Each type of treatment or drug has a different set of possible side effects. Your medical team should give you information about the side effects associated with any treatment they recommend for you. Ask for more information if you are worried about potential side effects. Your medical team can offer advice or prescribe medicines if you experience troublesome side effects during your lymphoma treatment.
Follow-up of nodal marginal zone lymphoma
When you are in remission (disappearance or significant shrinkage of lymphoma) after your treatment, or during a period of active monitoring (watch and wait), you have regular follow-up appointments in the clinic.
Your follow-up appointments are to check that:
- you are recovering well from treatment
- you have no signs of the lymphoma coming back (relapsing) or getting worse
- you are not developing any late effects (side effects that develop months or years after treatment).
At each appointment, your doctor examines you and asks if you have any concerns or symptoms. You might have blood tests. You are unlikely to have a scan unless you have troubling symptoms.
Relapsed or refractory nodal marginal zone lymphoma
It is common for nodal MZL to come back (relapse) after successful treatment. You can usually have more treatment to give another period of remission. This approach can often control the lymphoma for many years.
Several targeted drugs are being tested in clinical trials. Your doctor might ask you if you would like to take part in a clinical trial to help test new treatments and to find out what the best treatment is for nodal MZL that has come back or has not responded to previous treatment (refractory lymphoma). However, you are under no obligation to take part.
If you don’t want to take part in a clinical trial, or if there isn’t one that is suitable for you, you are likely to be treated with rituximab in combination with chemotherapy. You might be given the same treatment that you had before, or a different type of treatment. Your doctor will consider how you responded to your previous treatment, your general health and your personal preference before making a final recommendation on your treatment plan.
Very occasionally, your medical team might recommend that you have a stem cell transplant using your own stem cells (an ‘autologous’ stem cell transplant). Stem cell transplants are usually only considered for nodal MZL if you have lymphoma that relapses very soon after chemo-immunotherapy. Stem cell transplants are a very intense form of treatment and you have to be fit enough to have one. A stem cell transplant allows you to have very high doses of chemotherapy. It might give you a better chance of having a long-lasting remission (no evidence of lymphoma) than standard chemotherapy regimens.
Research and targeted treatments
Nodal MZL is rare so most clinical trials include people with nodal MZL alongside other types of low-grade lymphoma.
There are several types of treatment being tested in clinical trials for marginal zone lymphomas, including drugs already approved for other types of lymphoma. These include:
- B-cell receptor pathway inhibitors, such as BTK inhibitors, which block signals involved in the growth and survival of lymphoma cells
- proteasome inhibitors which disrupt the balance of proteins in lymphoma cells
- BCL-2 inhibitors which activate the process of natural cell death
- immunomodulators which change how your immune system responds to lymphoma cells
- antibody treatments which bind to proteins on the surface of lymphoma cells to help your own immune system destroy them
- CAR T-cell therapy which uses modified cells from your own immune system to fight lymphoma.
Some of these might be available to you through a clinical trial. If you are interested in taking part in a clinical trial, ask your doctor if there is a trial that might be suitable for you. To find out more about clinical trials or to search for a trial that might be suitable for you, visit Lymphoma TrialsLink.
