Skin (cutaneous) B-cell lymphoma
Skin (cutaneous) lymphomas are non-Hodgkin lymphomas that start in the skin. This information is about a rare type of skin lymphoma called B-cell skin lymphoma (also known as cutaneous B-cell lymphoma, or CBCL).
There are a few different types of B-cell skin lymphoma. This page contains information on all the different types. This might seem daunting. If you know what type of B-cell skin lymphoma you have, you may wish to read only the sections that apply to you.
On this page
Low-grade B-cell skin lymphoma
What is B-cell skin lymphoma?
Lymphoma is a cancer that starts in white blood cells called lymphocytes, which are part of your immune system. There are two types of lymphocyte: T lymphocytes (T cells) and B lymphocytes (B cells). B cells make antibodies which stick to proteins that the body recognises as foreign (antigens). T cells can either destroy cells in the body that are infected by antigens or activate other parts of the immune system to help. Lymphomas can develop from either T cells or B cells.
Skin lymphomas are lymphomas that develop in the skin and are not affecting any other areas of the body at the time they are diagnosed. B-cell skin lymphomas are skin lymphomas that develop from B cells.
We have separate information on T-cell skin lymphomas (skin lymphomas that develop from T cells).
A lymphoma that starts somewhere else in the body and then spreads to the skin is not a skin lymphoma. If you have a lymphoma that has spread to the skin, our information on the particular type of lymphoma will be more relevant for you.
Who gets B-cell skin lymphoma?
B-cell skin lymphoma (also called cutaneous B-cell lymphoma or CBCL) is rare. Only around 100 people are diagnosed with B-cell skin lymphoma in the UK each year.
Scientists don’t know exactly what causes skin lymphoma but there are some factors that might increase your risk of developing it. These vary according to the type of skin lymphoma.
- Age: B-cell skin lymphoma is more common in older people, over the age of 75.
- Sex: Women are around twice as likely to develop B-cell skin lymphoma than men.
- Infections: There is a link between B-cell skin lymphoma and an infection called Borrelia burgdorferi. This infection is spread by ticks and is the cause of Lyme disease. Your doctor is likely to test you for Borrelia burgdorferi, but most people with B-cell skin lymphoma do not have it.
Symptoms of B-cell skin lymphoma
The main symptom of B-cell skin lymphoma is a lump, or lumps, in the skin. The lumps often appear as small, raised, solid areas of skin that can look like small pimples. These are called papules. They may develop into thickened but still quite flat areas called plaques, or larger lumps, often deep red or purplish, called nodules or tumours. Papules or nodules appear most commonly on the head, neck, back or legs.
It is important to remember that B-cell skin lymphomas are rare. There are many skin conditions that may look similar but are not lymphomas.
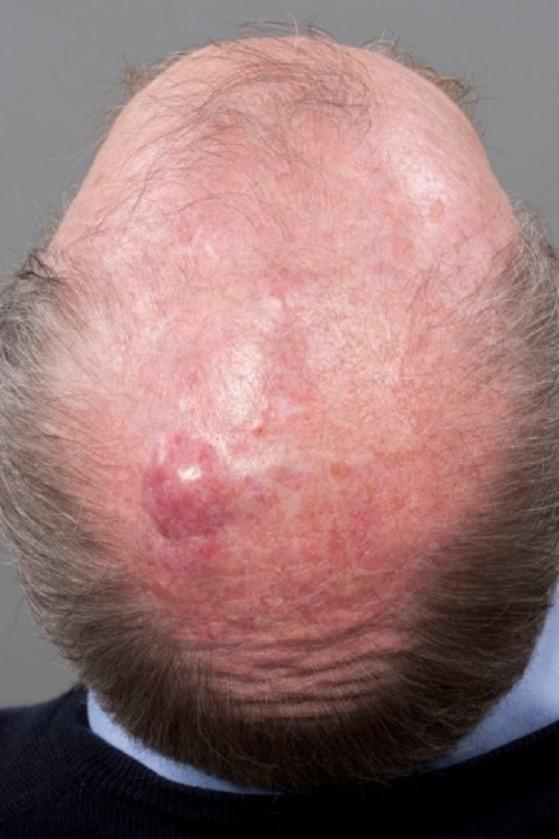
You might have one lump or plaque, or you might have several, which may be grouped together or more widely spread out. Sometimes the lumps break down (ulcerate) and may become infected. Speak to your medical team if this happens.
For more information about these symptoms, including photographs, see our overview of skin lymphomas.
You might also have swollen lymph nodes in your neck, armpits or groin. They may be inflamed as a reaction to the nearby skin irritation or because they contain abnormal lymphoma cells.
A few people experience more general symptoms of lymphoma such as unexplained weight loss, fevers or night sweats. However, this is quite uncommon with B-cell skin lymphoma.
Many skin lymphomas develop very slowly, over months or years. They can look like more common skin conditions, such as eczema or psoriasis, or reactions to insect bites or vaccinations. Because of this, it may take a long time for your GP to rule out other conditions and refer you to a specialist. This might be a specialist in skin diseases (dermatologist) or a specialist in diseases of the blood and lymphatic system (haematologist).
Diagnosis and staging
B-cell skin lymphomas are diagnosed using a procedure called a skin biopsy. A skin biopsy can find out the exact type of skin lymphoma you have and whether it is low-grade (slow-growing or indolent) or high-grade (fast-growing or aggressive). However, diagnosing skin lymphoma is not always straightforward, even for a specialist. You might need several skin biopsies before your doctor is able to confirm your diagnosis.
I told my GP about some itchy lumps on my upper arms. He dismissed them as nothing more than fatty tissue. The following year, I was referred to my local hospital where the lumps were cut out and sent for analysis. My next hospital appointment was with an oncologist who acknowledged that I had cancer – a low grade non-Hodgkin Lymphoma.
You might also have other tests to find out if any other parts of your body are affected by lymphoma – this is called ‘staging’. These tests may include:
- a physical examination
- blood tests to look at your general health and to test for bacterial or viral infections that might be linked to your lymphoma
- a CT scan or PET/CT scan
- a bone marrow biopsy
- a lymph node biopsy (if you have swollen lymph nodes).
Waiting for the results of your tests can be difficult, but it is important that your specialist knows exactly what type of lymphoma you have so they can give you the most appropriate treatment.
A diagnosis of B-cell skin lymphoma can take a long time and not only affects the person with the diagnosis, but can also have an impact on your family, friends and carers.
Staging of B-cell skin lymphoma
The stage of the lymphoma describes how far it has grown. The stage, along with the particular type of lymphoma you have, helps your medical team decide on the most appropriate treatment for you. For B-cell skin lymphomas, the stage of your lymphoma when it is diagnosed does not affect your outlook (prognosis).
If your lymphoma is only affecting your skin, it might be staged as a lymphoma that has started outside the lymphatic system (an ‘extranodal’ lymphoma) but has not spread anywhere else. This is known as Stage 1E. Doctors might add an ‘A’ after it (Stage 1AE). This means you do not have any symptoms known as ‘B symptoms’ (unexplained weight loss, fevers or night sweats).
Otherwise, B-cell skin lymphomas are staged using a system called ‘TNM’. TNM stands for:
- Tumour: how many papules, nodules or tumours you have, how big they are and where they are. This is shown by a ‘T’ and a number between 1 and 3, sometimes followed by a letter between a and c.
- Nodes: how many lymph nodes are involved (if any) and where they are. This is shown by an ‘N’ and a number between 0 and 3.
- Metastasis: whether the lymphoma has spread (metastasised) to any part of the body apart from your skin or lymph nodes. This is shown by an ‘M’ followed by 0 or 1.
Your stage includes all three measures. For example:
- A person with one skin nodule smaller than 5cm, no swollen lymph nodes and no lymphoma anywhere else in their body would have a stage of T1aN0M0.
- A person with several skin nodules confined to a 30cm area of skin, swollen lymph nodes in two areas of their body but no lymphoma anywhere else would have a stage of T2bN2M0.
Staging helps monitor changes in your lymphoma over time. This can help your doctors decide on the best treatment for you.
Types of B-cell skin lymphoma
There are three main types of B-cell skin lymphoma. They have technical names based on what the lymphoma cells look like under a microscope. The different types behave differently and may be treated differently.
- Primary cutaneous follicle centre lymphoma is the most common type of B-cell skin lymphoma. It is a low-grade lymphoma. It typically develops in people in their 50s and is slightly more common in men than women.
- Primary cutaneous marginal zone lymphoma is also a low-grade lymphoma. It typically develops in adults aged 35 to 60 years old and is slightly more common in men than women. Some cases are linked to an infection with a bacterium called Borrelia burgdorferi. This is carried by ticks and causes Lyme disease. However, most people with Lyme disease do not develop skin lymphoma.
- Primary cutaneous diffuse large B-cell lymphoma, leg-type, is a very rare, high-grade lymphoma. It typically develops in people over 70 and is twice as common in women as men.
Low-grade B-cell skin lymphomas
Most types of B-cell skin lymphomas are slow-growing (low-grade). Here, we outline the two main types of low-grade B-cell skin lymphoma, and the treatment for them.
Primary cutaneous follicle centre lymphoma
Over half of all B-cell skin lymphomas are primary cutaneous follicle centre lymphoma. It is a low-grade lymphoma that develops over months or years. It usually appears as pink, reddish or purple papules, plaques or nodules, most commonly on the head, neck, chest or back. It often develops as a single lesion but you might have several lesions, usually grouped together.
Primary cutaneous marginal zone lymphoma
Primary cutaneous marginal zone lymphoma is another low-grade lymphoma. It is also known as ‘extranodal marginal zone lymphoma of mucosa-associated lymphoid tissue’ (MALT lymphoma). It usually appears as pink, red or purplish papules, plaques or nodules that develop on your arms, chest or back, or sometimes your legs. They can develop in one place or in several places and are very slow-growing.
Treatment of low-grade B-cell skin lymphomas
If you have primary cutaneous marginal zone lymphoma and your blood tests show you have an infection with Borrelia burgdorferi, you have treatment with antibiotics first. This might be the only treatment you need.
Otherwise, all types of low-grade B-cell skin lymphoma are treated in the same way.
- You might have low dose superficial radiotherapy on and around the margin of the lymphoma after diagnosis. In many cases this might be all the treatment you need.
- If only one, small area of skin is affected by lymphoma, you might have surgery to remove it. This may be followed by radiotherapy to prevent it coming back (relapsing).
- If just a few areas of your skin are affected, you usually have radiotherapy on its own. Surgery is not usually used for more than one site.
- Sometimes the lesions associated with low-grade B-cell skin lymphomas can resolve themselves spontaneously.
If your lymphoma is more widespread, localised radiotherapy or surgery are generally not suitable. Treatment depends on how much of your skin is affected and whether the lymphoma has spread anywhere else.
- If you have lymphoma in several areas of your skin but you are not experiencing any troublesome symptoms, you might not need treatment straightaway. Instead, your doctor might monitor your progress. This is called active monitoring, or ‘watch and wait’. It does not mean there is no treatment for you, but that you would not benefit from starting treatment straightaway. This saves you experiencing side effects of unnecessary treatment. You have treatment when you need it.
- If you have lymphoma in several areas of your skin and you are experiencing symptoms, you might have a chemotherapy drug called chlorambucil or an antibody treatment called rituximab. This can be given through a drip into a vein (intravenously) or as an injection directly into the affected skin.
- If your lymphoma has spread to your lymph nodes or other parts of your body, you might have rituximab plus a chemotherapy regimen (combination of treatment) such as bendamustine or CVP (cyclophosphamide, vincristine and prednisolone).
If your lymphoma comes back (relapses) after treatment, it can often be successfully treated with the same treatment you had the first time.
There is more information on our page on treatment of skin lymphoma.
High-grade B-cell skin lymphomas
There is one main type of B-cell skin lymphoma that is fast-growing (high-grade). Here, we outline this type, and how it might be treated.
Primary cutaneous diffuse large B-cell lymphoma
Primary cutaneous diffuse large B-cell lymphoma, leg type, is a high-grade skin lymphoma. It typically develops as one or more large, bluish-red nodules that grow rapidly over a few weeks or months. They are usually on the lower legs but around 1 in 10 nodules develop in other places. They can become quite large and deep and they may break down (ulcerate).
Treatment of high-grade B-cell skin lymphomas
Primary cutaneous diffuse large B-cell lymphoma, leg type, is usually treated with chemotherapy, often followed by radiotherapy to the affected area. The chemotherapy regimen (combination of treatment) most commonly used is called CHOP and is usually given alongside an antibody treatment called rituximab (R-CHOP):
- cyclophosphamide
- hydroxydaunorubicin
- vincristine, also known as Oncovin®
- prednisolone.
If you are not well enough to have chemotherapy, you might have radiotherapy on its own to help control your symptoms. Some people have rituximab on its own.
If the lymphoma comes back (relapses), your doctor will probably suggest more chemotherapy.
There is more information on our page on treatment of skin lymphoma.
Outlook
Your outlook (prognosis) depends on lots of factors, including your age and general health and the exact type of skin lymphoma you have. Your specialist is best placed to advise you on your outlook based on your individual circumstances.
In general, low-grade B-cell skin lymphomas have an excellent outlook. They are often diagnosed early, grow slowly and respond well to treatment. Any skin problems they cause come and go and only need treatment some of the time.
Some low-grade lymphomas do not become obvious until they are more advanced and the disease has spread to the lymph nodes, blood or internal organs. With treatment, many people with advanced low-grade skin lymphoma have long periods when they are free of symptoms.
Primary cutaneous diffuse large B-cell lymphoma, leg type, is a high-grade lymphoma and is more aggressive in its behaviour. It needs more intensive treatment more urgently. Most people respond to treatment but it is more likely to come back (relapse) than low-grade B-cell skin lymphoma.
Occasionally, low-grade B-cell skin lymphomas can change (transform) into a faster-growing type, although this is very rare. Your medical team should check for this. If your lymphoma transforms, you need more intensive treatment.
Follow-up
How often you have check-ups after your treatment ends depends mainly on what type of skin lymphoma you have and how it is responding to treatment.
If your skin lymphoma is fast-growing (high-grade), or is continuing to grow, you may see your doctor every 4 to 6 weeks.
You might only see your specialist every 6 to 12 months if:
- you have a low-grade skin lymphoma
- your condition is stable (unchanging) or in remission (no evidence of the disease) after treatment.
At the clinic, your doctor will ask about your symptoms and examine you. Occasionally, you might have blood tests, scans or biopsies.
Tell your doctor if you have any symptoms that are troubling you, if you’ve noticed any changes in your skin, or you have any new swellings.
Research and clinical trials
Researchers are continually trying to find out which treatment or combination of treatments work best for skin lymphomas. Your doctor may ask you to consider taking part in a clinical trial. Clinical trials allow new treatments to be evaluated and compared with more established ones. Studying treatments is the only way that new and, hopefully, better treatments can become available.
Find out more about clinical trials and search for a trial that might be suitable for you at Lymphoma TrialsLink.
