Thrombocytopenia (low platelets)
Thrombocytopenia is a shortage of platelets in your blood. Platelets help your blood clot when you injure yourself. Thrombocytopenia can make you more likely to bruise or bleed.
On this page
What causes thrombocytopenia in people with lymphoma?
What is thrombocytopenia?
Thrombocytopenia is a shortage of platelets in your blood.
Platelets are a type of blood cell that help your blood to clot. When you cut yourself or damage a blood vessel, platelets stick together to make a ‘plug’ that blocks the hole. They also activate proteins in your blood called clotting factors, which help stop any bleeding.
Platelets are made in your bone marrow (the spongy centre of larger bones). They are very short-lived: they only stay in your bloodstream for 5 to 10 days before they are removed by your spleen. Your bone marrow works all the time to make new platelets to replace the ones that are lost. It works harder if you are bleeding somewhere in your body and you need platelets to help stop it.
If you have a low number of platelets, your medical team might say that you are thrombocytopenic.
What causes thrombocytopenia in people with lymphoma?
You might develop thrombocytopenia if your bone marrow is not making enough platelets, or if your platelets are being used up faster than your bone marrow can make them.
In people who have lymphoma, common causes include:
- Lymphoma in the bone marrow. If you have lymphoma cells in your bone marrow, they take up space that is normally used to make healthy blood cells. This can lower the number of platelets your bone marrow makes, and might lead to thrombocytopenia. Thrombocytopenia caused by lymphoma in your bone marrow often improves once you start lymphoma treatment.
- Lymphoma treatments. The aim of lymphoma treatment is to kill lymphoma cells, but a side effect of many types of lymphoma treatment is that some healthy cells are also destroyed. This can include the cells in your bone marrow that make new platelets. If these cells don’t make enough platelets to replace the ones that die off naturally, your platelet count falls. Thrombocytopenia due to chemotherapy usually develops 7 to 10 days after treatment and typically recovers after a week or so. Thrombocytopenia due to radiotherapy might take longer to recover from, depending on the part of your body being treated, the dose and how long you are treated for. It gradually recovers over weeks or months.
- Platelets collecting in a swollen spleen (splenomegaly). Some platelets are stored in your spleen. If your spleen is affected by lymphoma, it can become very swollen. If your spleen is bigger than normal, more platelets collect there. This leaves fewer platelets than normal in your bloodstream.
- Immune thrombocytopenia. Sometimes, lymphoma cells make antibodies that attack your own cells. These are called autoantibodies. If these autoantibodies stick to platelets, the platelets are destroyed when they pass through your spleen. If your bone marrow can’t make platelets fast enough to replace the ones that are destroyed, your platelet count drops and you develop thrombocytopenia. This type of thrombocytopenia is called ‘immune thrombocytopenia’. It is rare in people with Hodgkin lymphoma and most types of non-Hodgkin lymphoma, but it can affect up to 1 in 10 people with chronic lymphocytic leukaemia (CLL).
- Other causes which might or might not be related to your lymphoma, including:
- certain infections
- alcohol dependence
- liver disease
- some antibiotic and antiviral medicines
- certain genetic conditions.
What are the symptoms of thrombocytopenia?
Most people with a low platelet count don’t have any symptoms. This is because your body has a built-in reserve with many more platelets than you need for day-to-day life.
If your platelet count falls to very low levels, you might notice some symptoms and signs. In general, the lower your platelet count, the stronger the symptoms. Symptoms can include:
- bruising more easily than usual
- bleeding for longer than usual after a cut
- bleeding after minor injuries that wouldn’t normally bleed.
If you have a low platelet count that causes bleeding, you might also develop anaemia.
Contact your medical team if you develop any of the following symptoms:
- nosebleeds
- bleeding gums after brushing your teeth
- heavier or longer periods than is usual for you
- bleeding for longer than you’d expect after a cut or scratch
- bruising more easily than usual
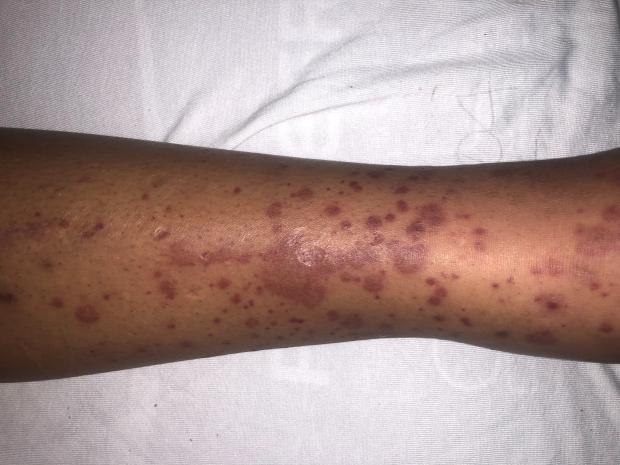
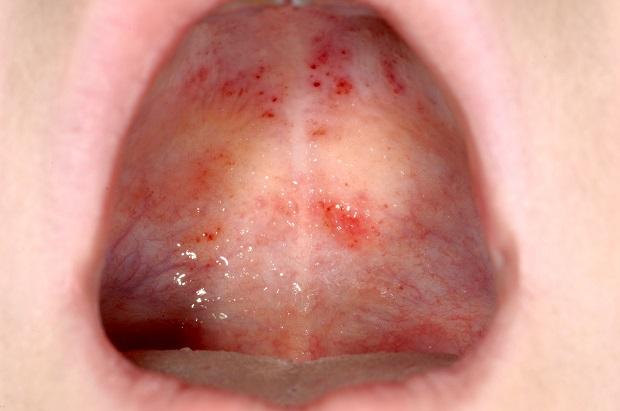
- red or purple patches or spots called ‘purpura’ or ‘petechiae’ on your skin (often on your legs), your lips or in your mouth (see photos below)
- blood in your sick (vomit)
- blood in your wee
- blood in your poo (this might be obvious, bright red blood or it can make your poo black and sticky)
- painful joints
- persistent headache, blurred vision or a change in your level of consciousness.
If you start bleeding, get in touch with your hospital straight away.
How is thrombocytopenia diagnosed?
The number of platelets in your blood is measured by a blood test called a full blood count (FBC).
Thrombocytopenia means having a lower number of platelets than is usual for you.
Healthy adults usually have between 150 billion and 450 billion platelets in every litre of blood. This is usually written as 150 to 450x10^9/L. Doctors and nurses usually just refer to the number (for example, a platelet count of 150 means 150 billion platelets per litre of blood).
How is thrombocytopenia treated?
Thrombocytopenia often gets better on its own quite quickly, and many people with a low platelet count don’t need any treatment at all. However, if your platelet count is very low, or you are at particular risk of bleeding, you might need treatment.
If there is a particular cause for your low platelet level, such as an infection, your doctor will aim to treat that first. Other treatment options include:
- Changes to your medicines. Some medicines, such as some antibiotic and antiviral medicines, can cause thrombocytopenia. Other medicines, such as blood-thinning treatments and some drugs you can buy without a prescription (for example, aspirin or ibuprofen) can increase your risk of bleeding if you have thrombocytopenia. Your medical team will check what medicines you are taking and will stop or adjust the dose of any that might be affecting your platelet count or your risk of bleeding. If you are having chemotherapy and your platelets are very low, your chemotherapy dose might be reduced, or you might have a longer break between treatment cycles to give your platelet count time to recover. Sometimes, your chemotherapy regimen might be changed.
- Platelet transfusion. A platelet transfusion involves having platelets from a healthy donor through a drip into one of your veins. Platelet transfusions aim to increase your platelet count enough to stop any bleeding or to reduce your risk of bleeding. The effect of a platelet transfusion only lasts for a few days because the platelets get used up. You might need a platelet transfusion if:
- you have an extremely low platelet count (less than 10)
- you have a very low platelet count (less than 20) and a fever (temperature above 38°C)
- you have a low or very low platelet count (less than 30 to 50) and you are bleeding
- you have a low platelet count (less than 50 to 100) and you need to have an operation or other medical procedure that puts you at risk of bleeding.
- Treatments for immune thrombocytopenia. If your thrombocytopenia is caused by autoantibodies destroying your platelets, platelet transfusions usually do not help. Instead, the treatment for this type of thrombocytopenia aims to reduce the number of autoantibodies being made, or stop your platelets being destroyed. In some cases, treating your lymphoma is also effective at treating immune thrombocytopenia. Other treatment options include:
- steroids, which reduce the activity of your immune system
- immunoglobulin replacement therapy, which stops cells in your spleen destroying platelets
- rituximab, which targets the cells that make antibodies
- having your spleen removed (splenectomy)
- treatment with other drugs that dampen your immune system (immunosuppressants)
- treatment with a thrombopoeitin receptor agonist to encourage your bone marrow to make more platelets.
- Treatment to help your blood clot. If you are bleeding, or you need to have a procedure that puts you at risk of bleeding, you might need other treatments to help your blood clot, such as:
- tranexamic acid, which helps prevent bleeding by stopping blood clots from being broken down
- an injection of vitamin K, which your body needs to make proteins that help blood clot (clotting factors)
- fresh frozen plasma (the liquid part of blood, which contains clotting factors) from a healthy donor given through a drip into one of your veins.
Reducing your risk of bleeding
If you have very low platelet levels, there are some precautions you can take to reduce your risk of bleeding.
Food, drink and medicines
- Try to limit how much alcohol you drink as it can make bleeding worse.
- Check with your doctor before taking any over-the-counter medicines, supplements or herbal remedies.
- Do not take aspirin or other blood-thinning medicines unless your doctor has told you to.
- Avoid using enemas or suppositories.
Activities
- Be very careful when you use knives, scissors or other sharp tools.
- Avoid high-impact sports (for example, running or football) and contact sports (for example, rugby or martial arts).
- Wear gloves and clothes that cover your skin to help protect you from scratches and cuts if you do activities where you might injure yourself (such as gardening, crafts or DIY).
- Wear shoes or slippers to protect your feet from injuries.
Hygiene
- Brush your teeth gently using a soft toothbrush. Avoid flossing to prevent your gums bleeding.
- Be gentle when blowing your nose to help prevent nosebleeds.
- Use an electric razor instead of wet shaving.
- Use sanitary towels instead of tampons.
- Use a water-based lubricant during sex. (You might be advised to avoid sex completely if your platelet count is very low.)
What to do if you start to bleed
- Stay calm.
- Sit down or lie down.
- Apply pressure to the injury if you can.
- Use an ice pack to slow the bleeding.
- If possible, raise the injury above the level of your heart.
- Contact your hospital.
