MRI scan
MRI stands for magnetic resonance imaging. MRI scans use strong magnetic and radio waves to make detailed cross-sectional images of the inside of your body.
We have separate information about being referred for tests and scans, CT and PET/CT scan, ultrasound and X-ray scans, and waiting for test results. You might also be interested in our video about scans for lymphoma.
On this page
What is an MRI scan?
An MRI scanner is a machine that contains strong magnets. It uses these magnets and radiowaves to make a detailed picture of the inside of your body. An MRI scan alone cannot diagnose lymphoma.
You can find out more about how MRI scans work on the Radiology info.org website.con
Will I have an MRI scan?
You might have an MRI scan if your medical team think you could have lymphoma in your:
brain and spinal cord (central nervous system)
- head and neck
- bones.
An MRI scan alone cannot diagnose lymphoma. The standard way to confirm a diagnosis is through a biopsy.
In some cases, doctors use an MRI instead of a computerised tomography (CT) or positron emission tomography (PET) scan. This might be the case if:
- you have an allergy to the contrast agents (a type of dye) that are used in CT and PET/CT scans
- you are pregnant.
Preparing for an MRI scan
Before the day of your scan, you’ll be given information about how to prepare for it. This includes about:
- Food and drink – you can usually eat and drink as normal on the day of your scan. Your medical team will tell you if this is not the case. For example, you might be given separate advice if you have diabetes.
- Medication – your medical team should tell you if it’s safe to have any of your usual medication before your scan. If you are taking medication for diabetes, they might advise you not to take tablets or insulin for a number of hours before the scan.
On the day of your scan:
- You will be asked to take off any metal you’re wearing, for example, items with a zip, jewellery, a belt, watch, or underwired bra.
- If you wear glasses, you might need to remove these.
- It’s usually OK to wear prescription, non-coloured contact lenses. However, you are likely to be told not to wear any coloured or cosmetic contact lenses as they might contain metal.
- The staff in the scanning department ask you whether you are, or could be, pregnant.
- You might be given a contrast agent.
- It’s a good idea to empty your bladder before you have the scan because you’ll need to lie still for a long time.
If you have any questions about your scan before the day, contact the hospital.
I am aware that some people feel unnerved by being in a confined space in the scanning machine. I found it best to close my eyes and imagine myself elsewhere. I felt that if it helps the team make the correct diagnosis and organise the best treatment, it is worth it.
Contrast agents
A contrast agent is a type of dye. It helps to show structures inside your body (blood vessels, organs and tissues) clearly. This can help to improve the quality of the scan image.
Most commonly, MRI scans use either:
- gadolinium, by injection
- barium sulfate, as a drink.
Doctors choose the most suitable type of contrast agent for you based on which part of your body needs to be scanned.
If you have a contrast agent by injection, it can sometimes sting where the needle goes in. You might feel warm or cold where the contrast agent is injected.
Depending on the type of contrast agent, you might experience the following:
- warmth travelling down your arms
- a strange taste in your mouth
- feeling as though you need to wee
- feeling sick or dizzy.
These usually pass within a few minutes.
Allergic reactions
There is a small risk of having an allergic reaction to a contrast agent. Staff monitor you carefully and are trained to treat any allergic reactions quickly.
In general, allergic reactions to contrast agents are mild. However, in more severe cases, they could cause itchy skin, swollen lumps and breathing difficulties.
Before you have the contrast agent, hospital staff check your medical notes and ask you whether you have:
- certain conditions (for example kidney problems)
- particular allergies
- had an allergic reaction to a contrast agent in the past.
These factors could increase your risk of developing an allergic reaction to the contrast agent so you might have your scan without one.
Having an MRI scan
You usually have an MRI scan as an outpatient unless you are already staying in hospital. Not all hospitals have an MRI machine so you might have to travel to a larger centre for your scan.
An MRI scan usually takes around an hour. Your appointment might be longer if you need to have a contrast agent.
An MRI scan can take a long time and you do have to keep still. It can be very noisy too – I thought it sounded a bit like being inside a washing machine. I found relaxation techniques were really helpful. For example, you could imagine yourself somewhere else, like being on a beach or in a garden. When I was having an MRI scan, I used to focus my mind by imagining I was packing for a holiday – I went through every step in detail to keep myself occupied.
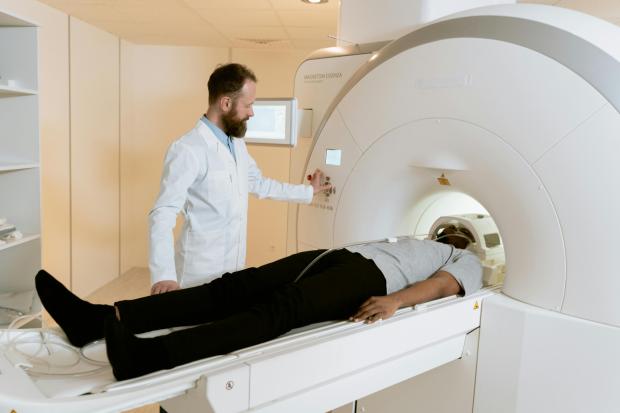
An MRI scanner is a large cylinder. It looks a bit like a tunnel or tube and it’s open at both ends.
- You lie on a couch that moves slowly into the scanner. Some people don’t like to be in the closed-in space. The staff are used to this and can offer support if you find it difficult.
- The hospital staff leave the room, but they can see you all the time through a window and a video camera. You can speak to one another through a two-way speaker.
- You need to keep very still during the scan.
- It can be quite hot and noisy in the scanner. You might feel vibrations and slight movement of the couch during the scan. You should be offered earplugs and you might be able to listen to music.
You can go straight home after the procedure. You shouldn’t drive if you have had a contrast agent or a sedative (drug to relax you).
You might be interested in Cancer Research UK's video about what it’s like to have an MRI scan.
©Cancer Research UK [2002] All right reserved. Information taken 01 May 2024
Frequently asked questions about MRI scans for lymphoma
Below are some questions people often ask about MRI scans and lymphoma. Speak to your medical team for advice specific to your situation.
Who carries out the scan?
A radiographer carries out the scan.
Can I take someone with me to my scan?
You can take someone, such as a friend or family member, to the hospital with you. However, for most scans, they will need to wait in a different room while you have your scan.
Will I be radioactive after the scan?
You will not be radioactive (giving off radiation) after your scan, so you do not need to take any precautions in being around other people.
Are MRI scans safe?
MRI scans are generally safe for most people, including during pregnancy. However, if you have metal in your body, doctors will need to think about whether it’s safe for you to have an MRI scan.
Talk to your medical team if you have questions about the safety of MRI.
The NHS website has more information about who can and can’t have an MRI scan.
Having metal in your body
If you have any metal in your body, doctors will first need to assess whether it is safe for you to have an MRI scan. This includes if you have metal in a pacemaker, hip replacement, implantable defibrillators, ear (cochlear) implants, staples from surgery and metal clips and plates put in after an injury. The strong magnetic fields MRI scans use could affect these. Your doctors will find out more about the type of metals in your body and decide on whether it’s safe for you to have an MRI scan.
Some tattoos have traces of metal in them, but most are safe in an MRI scanner.
Can I have a scan if I am pregnant or breastfeeding?
MRI scans are generally considered to be safe during pregnancy. However, doctors often avoid giving an MRI scan during the early stages (first trimester) of pregnancy. If possible, you’ll be advised to wait until later in your pregnancy before having an MRI scan.
Breastfeeding does not put your baby at risk.
Are scans painful?
MRI scans aren’t painful. However, some people find them uncomfortable if they need to stay still for a long time.
If you think you’ll find it difficult to lie still for long enough, talk to your doctor or another member of hospital staff before the day of your scan. They might suggest using support pillows to help keep you as comfortable as possible. In some cases, they might suggest that you take pain relief medication beforehand if lying still is likely to cause you discomfort. You could also talk to the radiographer on the day to help you find the most comfortable position for you.
What should I do if I feel anxious about having a scan?
Talk to a member of your medical team if you feel anxious about having a scan. They can answer any questions you have and might suggest ways of coping with your anxiety.
If you feel very anxious, you might be able to have an anti-anxiety drug before your scan. If you think this could help you, talk to the staff in the scanning department before the day of your appointment. If you have an anti-anxiety drug, you should not drive for the rest of the day so you might need to arrange transport home from your scan.
Can I have a scan if I have diabetes?
If you have diabetes, you might be given specific advice about what to eat on the day of your scan, including about how to take your medication. In some cases, your scan might be arranged for a time of day that plans around your usual blood sugar levels.
When will I get the results of the scan?
Your medical team should be able to give you an idea of when to expect your test results. Staff in the scanning department won’t be able to give you your scan results while you’re at the hospital.
The person doing the scan isn’t usually trained to understand what the images mean. Instead, this information needs to be sent to a specialist. The expert uses the scan and the results of all your other tests to help them work out what your scan pictures mean.
For some people, waiting for test results can be a particularly anxious time. Although the wait might feel long, it is important that doctors collect all of the information they need so that they can plan the best treatment for you. If you’d like to talk about how you’re feeling, our helpline team is here to support you.
Will I have scans during my follow-up?
You might have a scan at the end of your treatment to check how well your lymphoma has responded. Scans are not routinely used as part of follow-up as there is no evidence to suggest that follow-up scans for lymphoma change lymphoma treatment or outcomes.
